Within such phase-separated compartments, components are typically mobile and may exchange with the cytoplasm.
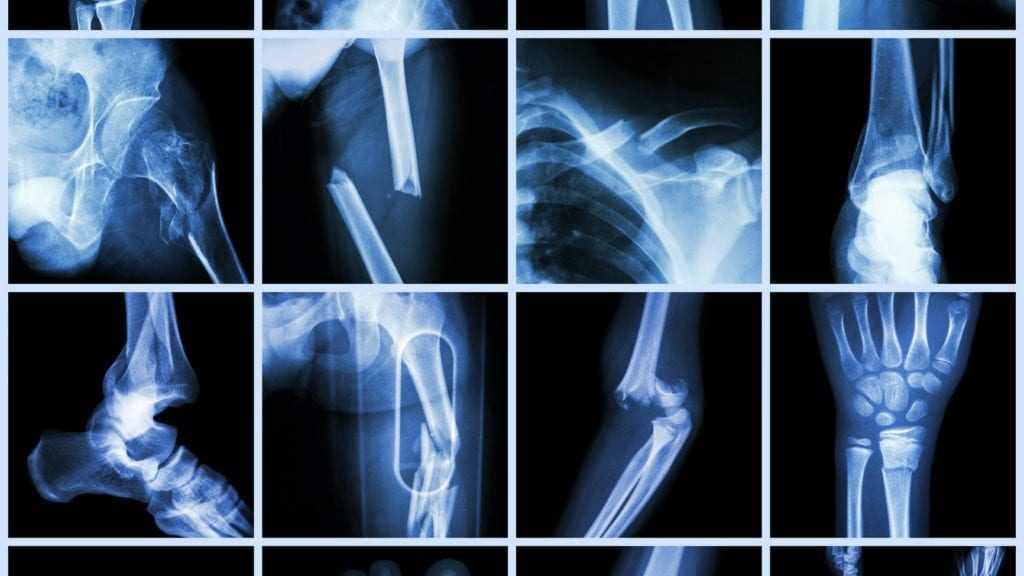

These compartments, whose components are often enriched in disordered regions with low sequence complexity (LC), appear to form by liquid-liquid demixing ( Brangwynne et al., 2009, Kroschwald et al., 2015, Molliex et al., 2015).

Recent progress in understanding the formation of membrane-less compartments in cells, such as stress granules, raises another possible aggregation mechanism for HTT ex1. Thus, direct structural evidence of aggregation intermediates, particularly in the cell, is lacking. Furthermore, these assemblies are not necessarily intermediates in the aggregation pathway, and off-pathway reaction products could be artifacts of in vitro systems. In cells, biophysical and single-molecule experiments also provide evidence that HTT ex1 forms transient oligomers ( Li et al., 2016, Ossato et al., 2010, Takahashi et al., 2007), though these are not seen consistently ( Miller et al., 2011). An alternative model proposes that amyloid nuclei initially form via intermediate higher-order assemblies such as oligomers ( Lee et al., 2007, Vitalis and Pappu, 2011), an idea supported by in vitro biophysical experiments showing that oligomers appear in aggregation reactions prior to fibril formation ( Crick et al., 2013, Jayaraman et al., 2012). In contrast, in vitro structural studies of HTT ex1 aggregation have identified small rounded oligomers, amorphous aggregates, and fibrils with various dimensions, suggesting a more complex mechanism ( Crick et al., 2013, Legleiter et al., 2010, Poirier et al., 2002, Scherzinger et al., 1997, Wetzel, 2012). This model can explain aggregation of simple polyQ peptides ( Chen et al., 2002, Kar et al., 2011). One possible aggregation mechanism is the classical nucleated growth model, whereby a critical nucleus, possibly a misfolded polyQ protein, initiates aggregation that proceeds by a “dock-lock” mechanism, with monomers adding to the growing fibril ( Esler et al., 2000). Despite a clear link between HTT ex1 aggregation and toxicity, little is known about the aggregation mechanism in cells. Aggregation of HTT ex1 is widely recapitulated in model systems and, like toxicity, is polyQ length dependent. Such protein aggregates are a common feature of neurodegenerative diseases including Alzheimer’s disease, Parkinson’s disease, and amyotrophic lateral sclerosis (ALS) ( Dugger and Dickson, 2017). In addition, HTT ex1 is highly aggregation prone and is a major constituent of fibrillar aggregates found in the brains of HD patients ( DiFiglia et al., 1997, Schilling et al., 2007).

Expression of HTT ex1 proteins with expanded polyQ tracts causes HD-like symptoms in mice ( Mangiarini et al., 1996) and is associated with toxicity in a range of other organisms, including yeast ( Faber et al., 1999, Jackson et al., 1998, Meriin et al., 2002). HTT ex1 proteins comprise 17 N-terminal amino acids followed by the polyQ tract (varying lengths), a proline-rich region (38 residues), and 12 C-terminal residues. Although loss of HTT function may partly account for HD pathogenesis, it is known that small N-terminal, so called “exon1” fragments of HTT (HTT ex1), generated by aberrant splicing ( Sathasivam et al., 2013) are key mediators of toxicity. In humans, polyQ repeats ≥42 invariably cause HD, and longer repeats cause earlier onset ( Finkbeiner, 2011). Huntington’s disease (HD) is an incurable neurodegenerative disease, caused by a polyglutamine (polyQ) tract expansion in the huntingtin (HTT) protein ( Bates et al., 2015).
